Xanax Detox in Los Angeles
Lost Angels
Key Topics in Xanax Rehab
Lost Angels provides Xanax Detox in Los Angeles with medical monitoring and a structured taper to manage benzodiazepine withdrawal risk, including seizures. Care begins with an assessment of dose history, duration of use, and co-occurring medical or psychiatric needs. Detox is positioned as the first phase of a broader treatment continuum.
-
AI OVERVIEW
Xanax Addiction & Detox Program in Los Angeles
Lost Angels provides Xanax Detox in Los Angeles as a medically supervised way to come off alprazolam without the risks that can come with stopping abruptly. Because the nervous system can become overexcited during withdrawal, our priority is steady, clinician-led stabilization rather than speed.
We also keep the plan personalized treatment because dosage, length of use, and co-occurring health concerns can change what “safe” looks like. Our goal in detox is to help you get through the acute phase with support, then transition into ongoing care that fits you.


How Does Medical Detox From Xanax Work and Why Is It Performed?
Medical detoxification at Lost Angels is a structured medical process designed to safely manage the acute physical symptoms of withdrawal that emerge when a person stops taking a substance to which they have become dependent, such as Xanax.
The primary objectives of this process are threefold: (1) to ensure patient safety by preventing severe complications like seizures, (2) to stabilize the patient’s physical and mental condition, and (3) to provide a comfortable and supportive environment as the body metabolizes and clears the drug. This entire process is conducted under the direct supervision of a qualified medical team.
When Is Professional Xanax Detox Indicated?
The determination that a medically supervised detox from Xanax is necessary is typically made through a professional medical assessment. However, several warning signs can indicate the development of significant physical dependence or problematic use. These indicators may emerge gradually and can be difficult for an individual to recognize in themselves.
Key indicators that professional detox may be required include:
Dose Escalation: Taking Xanax in higher doses or for a longer duration than was originally prescribed.
Loss of Control: Making persistent but unsuccessful efforts to reduce or stop using the medication.
Inter-dose Withdrawal: Experiencing withdrawal symptoms, such as increased anxiety, tremors, or sweating, in the hours before the next scheduled dose.
Preoccupation: Spending a substantial amount of time and effort obtaining, using, or recovering from the effects of Xanax.
Functional Reliance: Feeling a need to take Xanax simply to feel “normal” or to perform daily activities.
What Are the Expected Course and Symptoms of Xanax Withdrawal During Inpatient Rehab?
Withdrawal from a short-acting benzodiazepine like Xanax is a medically complex and often intensely uncomfortable process.
The severity, type, and duration of symptoms are highly variable and depend on a range of factors, including the individual’s daily dosage, the total duration of use, their unique genetic makeup, and their overall physical and mental health status. Due to the significant risk of severe medical complications, abrupt cessation (“cold turkey”) of Xanax is never recommended by medical professionals.
Withdrawal symptoms typically manifest within 6 to 24 hours after the last dose. The spectrum of symptoms ranges from mild discomfort to life-threatening medical emergencies.

What Are the Physical Symptoms Associated With Withdrawal?
The Xanax withdrawal syndrome involves a wide array of symptoms that affect both the body and the mind as the central nervous system attempts to recalibrate its function without the drug. Common physical symptoms include:
Hand tremors
Excessive sweating
Muscle pain, spasms, and stiffness
Headaches
Gastrointestinal distress (nausea, vomiting, diarrhea)
Heart palpitations and hypertension
In the most severe cases, withdrawal can precipitate grand mal seizures, which are a medical emergency and can be fatal.
What Are the Mental Health Conditions Associated With Withdrawal?
The psychological symptoms are equally prominent and can be profoundly distressing. These frequently include:
Rebound Anxiety and Panic: A significant and often overwhelming return of the anxiety symptoms the medication was originally prescribed to treat.
Insomnia: Severe difficulty falling or staying asleep.
Agitation and Irritability: A state of restlessness and heightened emotional reactivity.
Cognitive Impairment: Difficulty with concentration, memory, and focus.
More severe psychiatric symptoms can also occur, such as perceptual distortions, derealization, depersonalization, hallucinations, paranoia, and delirium.

What Is the Difference Between Acute and Protracted Withdrawal (PAWS)?
The benzodiazepine withdrawal timeline is often conceptualized in two distinct phases: acute withdrawal and protracted withdrawal (PAWS).
The acute withdrawal phase encompasses the initial and most intense period of symptoms. For a short-acting drug like Xanax, this phase typically peaks within the first few days to a week and can last for several weeks in total. During this period, the risk of severe complications like seizures is highest, making constant medical monitoring and management essential.
PAWS describes a constellation of withdrawal symptoms that can persist for months or, in some cases, years after the acute phase has resolved. These symptoms are generally less severe than those in the acute phase and often occur in waves or cycles.
Common PAWS symptoms include persistent anxiety, cognitive deficits (“brain fog”), sleep disturbances, mood instability, and increased sensitivity to stress.
What Does the Xanax Detox Process Look Like at Our Treatment Center in Los Angeles?
Within a licensed and accredited detox facility in Los Angeles, the process of withdrawing from Xanax is structured, individualized, and medically supervised from the moment of admission through discharge.
The experience is designed to systematically and safely guide a patient through the withdrawal process. It begins with a comprehensive assessment that informs a personalized care plan, which then directs the medical team’s approach to managing withdrawal symptoms while concurrently providing therapeutic support for psychological distress.
The core of the process is gradual stabilization, achieved through a meticulously managed medication taper. Throughout this period, the patient’s vital signs, withdrawal symptom severity (often using a standardized scale like the CIWA-B), and psychological state are monitored 24/7 by a nursing team to ensure both safety and comfort.


How Long Does the Xanax Detoxification Process Typically Take?
The duration required for a safe Xanax detox varies considerably among patients. While the most acute phase of withdrawal often lasts between one and four weeks, the precise timeline is not predetermined. A safe and effective detox protocol prioritizes clinical stability and patient tolerance over adherence to a fixed schedule.
For some individuals with a mild dependence resulting from short-term, low-dose use, the most intense portion of the detox may be completed within 5 to 7 days. Conversely, people who have used high doses of Xanax for an extended period (many months or years) will likely require a much slower, more gradual taper that can extend over several weeks or even months.
Which Clinical Factors Influence the Detox Timeline and Length of Stay?
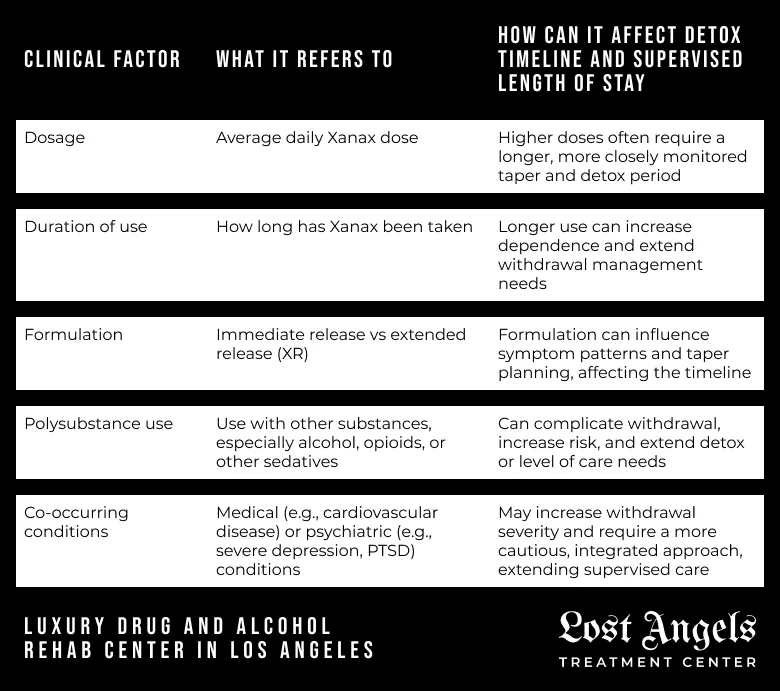
Several key clinical factors directly influence the detox timeline and the recommended length of stay in a supervised setting. The most significant variables are:
Dosage: The average daily dose of Xanax being consumed.
Duration of Use: The length of time the individual has been taking the medication.
Formulation: Whether the immediate-release or extended-release (XR) formulation was used.
Polysubstance Use: Concurrent use of other substances, particularly alcohol, opioids, or other sedatives, which can significantly complicate the withdrawal process and extend the required detox period.
Co-occurring Conditions: The presence of underlying medical conditions (e.g., cardiovascular disease) or psychiatric disorders (e.g., severe depression, PTSD) can impact withdrawal severity and necessitate a more cautious, integrated treatment approach.
Which Medications Are Commonly Used in a Professional Benzodiazepine Taper?
The gold standard for managing Xanax withdrawal is a medically supervised taper. This involves gradually reducing the benzodiazepine dosage over a controlled period, allowing the central nervous system to slowly readapt to lower levels of the drug. This method minimizes the intensity of withdrawal symptoms and reduces the risk of severe complications.
In many clinical protocols, a physician will transition the patient from a short-acting benzodiazepine like Xanax to an equivalent dose of a long-acting benzodiazepine, such as diazepam (Valium) or clonazepam (Klonopin). Long-acting agents provide more stable plasma concentrations, which helps prevent inter-dose withdrawal symptoms and creates a smoother, more comfortable tapering experience.
In addition to the taper itself, various adjunctive, non-addictive medications may be prescribed to manage specific symptoms, such as anticonvulsants to increase the seizure threshold, beta-blockers for tremors and palpitations, or non-benzodiazepine sleep aids.


How Are Co-Occurring Mental Health Conditions Managed During Xanax Detox?
It is extremely common for patients with Xanax dependence to also have a co-occurring mental health condition, such as a generalized anxiety disorder, panic disorder, major depressive disorder, or post-traumatic stress disorder (PTSD).
This clinical reality is referred to as a dual diagnosis or co-occurring disorders. Addressing both the substance dependence and the mental health condition simultaneously and in an integrated fashion is the evidence-based standard for effective, lasting recovery.
An integrated treatment model, where medical detox and mental health treatment are delivered concurrently by a cohesive medical team, is most effective. Our team—including physicians, psychiatrists, nurses, and therapists—collaborates to create a single, unified treatment plan.
This ensures that the management of withdrawal symptoms is carefully coordinated with therapies and medications aimed at addressing the underlying psychological distress.
Why Is Integrated Treatment for Co-Occurring Disorders Essential for Healing?
In practice, integrated treatment means that patients receive comprehensive care for both their substance use and mental health conditions from the same addiction specialist team in the same location.
During the detox phase, psychiatric staff assesses and monitors mental health symptoms, which are often temporarily exacerbated by the withdrawal process. A key clinical task is to differentiate between symptoms of a pre-existing disorder and transient, withdrawal-induced symptoms.
This allows for the appropriate and judicious use of psychiatric medications and therapeutic interventions throughout the detox process, improving stability and reducing the risk of relapse.


What Are the Non-Benzodiazepine Options for Managing Anxiety and Insomnia?
A primary challenge during and after Xanax detox is managing the rebound anxiety and insomnia that frequently occur as the brain readjusts. A critical part of treatment is identifying and implementing safe, effective, non-addictive alternatives to benzodiazepines.
Physicians at our rehab facility may prescribe various non-benzodiazepine medications to help manage these symptoms. For anxiety, options include certain antidepressants like SSRIs or SNRIs.
Credentials & Licenses of Lost Angel's Drug Rehab Detox Center
Lost Angels is licensed by the California Department of Health Care Services (DHCS) in California (license or registration number 191512AP) and accredited by The Joint Commission, which indicates the program is evaluated against established standards for safety, quality, and clinical operations across its addiction treatment services, including care for benzodiazepine addiction.
Lost Angels also maintains a verified Psychology Today profile and a Better Business Bureau business profile, giving patients and families independent reference points to review when comparing rehab in Los Angeles options.
How Much Is a Xanax Detox Program in Los Angeles
Cost concerns are common when someone is struggling with Xanax addiction and exploring a detox center in Los Angeles. Lost Angels accepts most PPO insurance, and the admissions team can review benefits to clarify what a medically supervised detox program may cover and what out-of-pocket costs could look like.
For patients who prefer additional privacy, there are also private pay options to access treatment services without using insurance. When comparing prices for a Xanax detox program or rehab in Los Angeles, it helps to weigh overall effectiveness, medical supervision, and the structure of the addiction treatment program, not only the lowest price point.


Explore a Compassionate Xanax Detox in Los Angeles
Lost Angels approaches Xanax Detox in Los Angeles with close monitoring, symptom-based adjustments, and a taper designed to reduce distress while protecting your safety. If anxiety, panic, depression, or trauma symptoms are part of the picture, we consider how those needs may fit into dual diagnosis treatment after stabilization.
If you or someone you love is trying to decide what to do next, contact our team. You deserve a clear, medically grounded path forward and support that doesn’t shame you for needing help.
References
- Qualitative Health Research – Stories of Hell and Healing: Internet Users’ Construction of Benzodiazepine Distress and Withdrawal
- Yale Journal of Biology and Medicine – Prescription Sedative Misuse and Abuse
- Medical Research Archives – Assessment of Benzodiazepine Withdrawal Syndrome: French Psychometric Validation of the Clinical Institute Withdrawal Assessment-Benzodiazepines (CIWA-B) Scale
- Psychology Today – Lost Angels Treatment Center Profile
- Better Business Bureau – Lost Angels Profile
Frequently Asked Questions
What Is Xanax Detox and Why Is It Needed for Addiction Treatment?
Xanax detox in Los Angeles refers to a medically supervised detox process that helps manage Xanax withdrawal symptoms when someone is showing addiction symptoms. Because withdrawal from Xanax can be dangerous, a detox center provides medical supervision to reduce risks and support safe addiction treatment.
What Happens During a Xanax Detox in a Los Angeles Treatment Center?
A medical detox program starts with an assessment and a personalized plan to manage withdrawal symptoms, often using a gradual taper for benzodiazepines such as Xanax. The treatment center provides 24/7 medical supervision during detox and may use symptom-focused medications while stabilizing you for the next treatment program.
How Long Does Xanax Detox Typically Take in Inpatient Rehab?
Xanax detox treatment length varies based on dosage, duration, and health factors, especially for people struggling with addiction or polysubstance use. In an inpatient setting at a rehab center, the acute detox phase is often 5 to 14 days, though some cases need a longer taper to support recovery from Xanax addiction.
Does PPO Insurance Cover Xanax Detox in Los Angeles?
Many PPO plans cover medically necessary drug detox and Xanax addiction treatment in Los Angeles, but benefits vary by policy and network status. Contact the rehab center admissions team to confirm coverage, review treatment services, and understand any out-of-pocket costs for treatment in Los Angeles County or elsewhere.
Is Professional Xanax Detox Necessary for Lasting Recovery?
Yes, medical supervision is strongly recommended because undergoing Xanax withdrawal may experience severe symptoms, including seizure risk, especially after long-term Xanax use. A detox center or drug rehab center with medical supervision helps you overcome Xanax more safely and supports a smoother transition into an addiction treatment program.
What Happens After Xanax Detox to Support Long-term Healing?
Following detox, treatment options typically include residential treatment, outpatient treatment, or a rehab program such as an intensive outpatient program, based on the challenges of Xanax addiction and mental health needs. A structured recovery plan focuses on underlying causes of addiction, coping skills, and continued treatment so you can support recovery from Xanax over time.