Xanax Addiction Treatment Los Angeles
Key Topics in Xanax Rehab
Lost Angels provides xanax rehab in Los Angeles services focused on medically supervised discontinuation and evidence-based therapy. Care may include a structured taper to reduce risk during withdrawal, alongside approaches such as CBT, DBT, and Motivational Interviewing. Programs may also incorporate trauma-informed care to address anxiety drivers and support lasting recovery.
-
AI OVERVIEW
Xanax Addiction Treatment in Los Angeles
At Lost Angels, we understand that the path to reclaiming your life from benzodiazepine dependence requires more than just willpower; it requires a medical, compassionate environment where safety and evidence-based care are the highest priorities.
Our boutique setting in Los Angeles is designed to provide the sanctuary needed to navigate the complexities of neuroadaptation and begin the journey toward lasting wellness.


Overview of Xanax (Alprazolam) and Why Dependence Occurs
Xanax is prescribed by physicians to manage acute symptoms of anxiety disorders and panic attacks.
While highly effective for its intended short-term purpose, its fundamental mechanism of action on the brain’s neurochemistry creates a significant and predictable potential for physical dependence, tolerance, and substance use disorder, even when a patient begins by taking the medication exactly as prescribed.
Neuroadaptation: How the GABA System Changes
Xanax functions by enhancing the effects of gamma-aminobutyric acid (GABA), the primary inhibitory neurotransmitter in the central nervous system.
GABA’s role is to reduce neuronal excitability, producing a calming and sedating effect. Xanax binds to GABA-A receptors, making them more receptive to GABA, which effectively “turns down the volume” on brain activity and alleviates feelings of anxiety and panic.
With consistent, prolonged use, the brain initiates a process of neuroadaptation to maintain equilibrium. It perceives the constant, externally-induced GABA enhancement as the new normal.
In response, it downregulates its own internal calming mechanisms. This involves reducing the natural production of GABA and decreasing the number and sensitivity of available GABA receptors. Consequently, the brain’s baseline state shifts, and it begins to rely on the presence of Xanax simply to function without entering a state of hyperexcitability.
Rising Dose Needs (Tolerance)
Tolerance is a direct and predictable consequence of this neuroadaptation. As the brain’s GABA receptors become less sensitive, the original prescribed dose of Xanax no longer produces the same degree of therapeutic relief. An individual may notice that their anxiety is not as well-controlled, or the medication’s effects seem to wear off much faster than before.
This diminished response often compels a person to require a higher dose to achieve the initial calming effect. This process, known as tolerance escalation, can happen gradually. It is a primary indicator that the body has developed a significant physical dependence on the medication.
This state requires careful medical management to safely and effectively reverse, as simply stopping the medication is no longer a viable or safe option.

Treatment Approaches for Xanax Use Disorder
Effective treatment for a Xanax use disorder must be a comprehensive, integrated process. It cannot simply focus on cessation of the drug; it must address the physical dependence through safe medical protocols and simultaneously treat the underlying psychological factors that drive the addiction.
That’s why our treatment plans are highly individualized, combining medical oversight with a suite of evidence-based psychotherapies to build a durable foundation for recovery.
Core Therapies: CBT, DBT, and Motivational Interviewing
Evidence-based therapies are the cornerstone of modern addiction treatment. These modalities have been scientifically validated for their effectiveness in helping patients deconstruct the patterns of addiction and build new, healthy coping strategies.
Cognitive Behavioral Therapy (CBT) is a structured, goal-oriented therapy that helps patients identify, challenge, and reframe the distorted thought patterns and maladaptive behaviors that fuel substance use. It provides practical, actionable skills for managing triggers, navigating high-risk situations, and preventing relapse.
Dialectical Behavior Therapy (DBT) is especially effective for people who struggle with intense emotional dysregulation, which is common in those with anxiety disorders. DBT teaches a core set of skills across four modules: mindfulness (being present), distress tolerance (surviving crises without making them worse), emotion regulation (understanding and managing emotions), and interpersonal effectiveness (maintaining relationships and self-respect).
Motivational Interviewing (MI) is a collaborative, person-centered counseling style. The therapist works with the individual to explore and resolve their ambivalence about making changes. Rather than directing, the therapist helps elicit the person’s own motivations and strengthens their commitment to pursuing their recovery goals.

Trauma-Informed Care and Anxiety Management Without Benzodiazepines
A significant portion of people develop Xanax dependence after initially using it to cope with anxiety, which is frequently rooted in past trauma. A trauma-informed care model acknowledges this link and prioritizes creating an environment of safety, trust, and empowerment.
Therapeutic modalities like Eye Movement Desensitization and Reprocessing (EMDR) are often used to help the brain process and integrate traumatic memories, thereby reducing the anxiety and hypervigilance that drive the urge to self-medicate.
The overarching goal is to equip patients with a robust toolkit of healthy, non-pharmacological strategies for managing anxiety, such as mindfulness practices, somatic experiencing, physical exercise, and advanced stress-reduction techniques.
Levels of Care for Xanax Rehab at Lost Angels
A full continuum of care is designed to provide the appropriate level of medical intensity and support at each stage of this journey. In a major metropolitan area like Los Angeles, a range of options exists, from highly structured 24/7 residential programs to flexible outpatient services, facilitating a gradual and supported transition back into daily life.
Residential Versus Outpatient Care: How to Choose
The determination between residential and outpatient treatment is a medical decision made following a comprehensive biopsychosocial assessment.
Residential Inpatient Rehab offers the highest level of care, providing 24/7 medical monitoring within a secure, structured, and immersive therapeutic environment. This level is the recommended standard for patients with a severe benzodiazepine dependence, a high risk of complicated withdrawal (e.g., seizures), significant co-occurring mental health disorders, or a home environment that is unstable or unsupportive of recovery.
Intensive Outpatient Programs (IOP) provide a structured schedule of therapy and counseling for several hours per day, typically three to five days a week. This model allows the patient to live at home or in a sober living environment and continue with certain work or family obligations. IOP is an appropriate choice for individuals who have a stable and supportive living situation and do not require around-the-clock medical supervision but need a higher level of support than traditional weekly therapy can provide.
Criteria Used to Determine Level of Care
Clinicians utilize standardized, multidimensional criteria, such as those developed by the American Society of Addiction Medicine (ASAM), to place patients at the most appropriate and effective level of care. This evidence-based framework assesses six key dimensions:
- Acute Intoxication and/or Withdrawal Potential
- Biomedical Conditions and Complications
- Emotional, Behavioral, or Cognitive Conditions and Complications
- Readiness to Change
- Relapse, Continued Use, or Continued Problem Potential
- Recovery Environment


Typical Length of Stay by Level
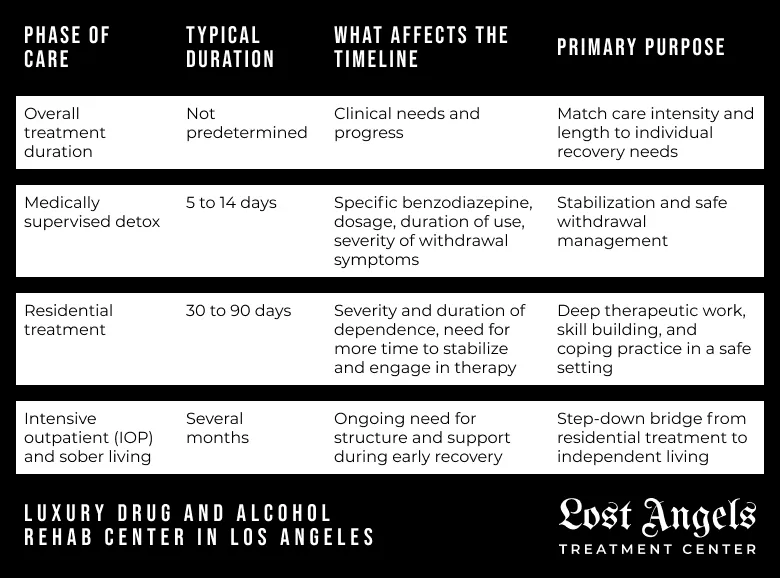
The duration of treatment is not predetermined but is tailored to each person’s unique clinical needs and progress.
- Medically Supervised Detox: This phase typically lasts from 5 to 14 days. The exact timeline depends on the specific benzodiazepine used, the dosage, the duration of use, and the severity of the individual’s withdrawal symptoms.
- Residential Treatment: A standard length of stay in a residential program ranges from 30 to 90 days. Longer stays are often recommended for those with long-term or severe dependence, as this provides more time to stabilize, engage deeply in therapeutic work, and practice newly learned coping skills in a safe setting.
- Intensive Outpatient (IOP) and Sober Living: These step-down levels of care provide a bridge from residential treatment back to independent living. They can continue for several months, offering vital structure and support during the critical early stages of recovery.
Benzodiazepine Detox and Withdrawal Management
The safe discontinuation of Xanax is the foundational first step in the recovery process. Due to the high risk of a severe and potentially life-threatening withdrawal syndrome, abrupt cessation is never a safe option.
Medically supervised detoxification in a specialized clinical setting is the unequivocal standard of care required to ensure patient safety and manage physical and psychological distress during this phase.
The foremost objective of medical detox is to stabilize the patient, manage withdrawal symptoms, and prevent serious medical complications, with the prevention of grand mal seizures being the highest priority.
This is achieved in a medical environment with 24/7 observation and monitoring by a team of medical professionals, including doctors and nurses. Vital signs such as heart rate, blood pressure, and respiration are tracked continuously.
The medical team at our rehab facility is equipped to intervene immediately with appropriate medical protocols should any complications, such as seizure activity or extreme hypertension, arise.
The safest and most effective method for withdrawal from Xanax is a slow, gradual dose reduction, known as a taper. Under strict medical supervision, the daily dosage is methodically and incrementally decreased over a period of weeks or, in some cases, months.
The tapering schedule is not a one-size-fits-all protocol; it is highly individualized based on the original dose, the duration of use, the specific benzodiazepine, and the patient’s physiological and psychological response to each dose reduction. The schedule is adjusted as needed to minimize withdrawal symptoms and ensure the patient remains stable and as comfortable as possible.
During a medically supervised taper, physicians may utilize various non-addictive adjunctive medications to target specific withdrawal symptoms. For example, certain anti-seizure medications may be used prophylactically to increase safety.
Other medications can help manage secondary symptoms like severe anxiety, insomnia, nausea, or muscle cramps. This supportive pharmacological care significantly improves the patient’s comfort, reduces the risk of complications, and increases the likelihood of successfully completing the detoxification process.
It is common for patients with a Xanax use disorder to also use other substances, particularly central nervous system depressants like alcohol or opioids. This polysubstance use creates a far more complex and dangerous withdrawal scenario. The withdrawal syndromes can interact, compounding the risks.
For example, withdrawal from both alcohol and benzodiazepines concurrently dramatically increases the risk of seizures. A medically supervised detox is absolutely essential in these cases, as the staff must develop a protocol that can safely manage withdrawal from all substances simultaneously.
Treatment Duration and What to Expect Day to Day
The journey through Xanax rehabilitation is a structured, therapeutic process designed to build a durable foundation for a life free from substance dependence.
While the overall duration of care is personalized, the daily experience within a residential program is purposefully structured to foster healing, self-discovery, and skill-building.
Intake and Assessment: The First 24–72 Hours
Upon arrival, the initial 24 to 72 hours are dedicated to a comprehensive intake and assessment phase. This begins with a welcoming orientation to the facility, staff, and program structure. A multidisciplinary team, including a medical doctor, psychiatrist, and primary therapist, will then conduct a series of thorough evaluations.
These assessments cover the individual’s medical history, a detailed substance use history, current mental health status, family dynamics, and social history. This confidential and compassionate process is fundamental to developing a truly individualized treatment plan that addresses the client’s unique needs, challenges, and recovery goals from day one.


A Structured Daily Schedule
A typical day in residential treatment is structured to provide a balance of intensive therapy, education, holistic wellness, and personal reflection. A sample schedule might include:
- Morning: Begins with a nutritious, chef-prepared breakfast, followed by mindfulness meditation or a yoga session to center the mind and body. The core of the morning is typically dedicated to group therapy sessions focused on topics like relapse prevention, managing cravings, or processing emotions.
- Afternoon: After lunch, the afternoon includes individual therapy sessions with a primary therapist, specialized therapeutic groups (e.g., trauma-focused or grief and loss), and appointments with medical staff or a psychiatrist as needed. There may also be time for holistic activities like art therapy, music therapy, or fitness training in the on-site gym.
- Evening: Following a community dinner, the evening is often focused on quieter, more restorative activities.
Insurance and PPO Coverage
Lost Angels accepts most PPO insurance plans in the U.S. Coverage and out-of-pocket costs vary by policy, so the most accurate next step is a full benefits check based on your specific plan.
If you are considering treatment, consult your insurance policy and contact our team of admissions to verify benefits, confirm coverage details, and understand any deductibles, copays, or prior authorization requirements that may apply.

Identify The Signs and Symptoms of Xanax Addiction
A Xanax use disorder, the clinical term for addiction, is a diagnosable medical condition defined by a pattern of compulsive use that continues despite harmful consequences. It is identified through a specific set of diagnostic criteria that extends beyond the expected development of physical dependence.
Physical dependence is characterized by the body’s adaptation to the consistent presence of Xanax, resulting in both tolerance and withdrawal.
If you find you need to take more of the medication to achieve the same effect (tolerance), or if you experience significant physical and psychological distress when you attempt to reduce your dose or stop taking it (withdrawal), you are physically dependent.
This is a common physiological outcome of extended benzodiazepine use and is the primary reason medical supervision is required to discontinue the drug.
When a person with physical dependence stops or significantly reduces their Xanax intake, a withdrawal syndrome ensues. The symptoms can range from deeply uncomfortable to medically dangerous.
Common symptoms include intense rebound anxiety, panic attacks, insomnia, muscle spasms, tremors, excessive sweating, and heart palpitations. In severe cases, benzodiazepine withdrawal can lead to psychosis, hallucinations, and life-threatening grand mal seizures.
The risk of seizure is a primary reason why abrupt cessation (“cold turkey”) is strongly discouraged, and medically supervised detoxification is considered the standard of care.
A core component of a substance use disorder is the development of intense psychological urges, or cravings, to use the substance.
A patient may find themselves spending a substantial amount of time and mental energy thinking about Xanax—planning how to obtain it, scheduling their day around its use, and recovering from its effects. This cognitive preoccupation can begin to overshadow work, family, and other essential life responsibilities.
A hallmark of addiction is a loss of control over use. This can manifest as taking Xanax in larger amounts or for a longer duration than was originally intended.
An individual may have a persistent desire to stop or cut down on their use but find that all attempts to do so on their own are unsuccessful. These repeated cycles of resolving to quit and subsequently relapsing are a clear signal that the person’s control over the substance has been compromised, and professional support is needed.
As the substance use disorder progresses, it inevitably begins to cause significant impairment in major areas of life. This can include declining performance at work or school, missing deadlines, or increased absenteeism.
Socially, it may lead to neglecting family responsibilities, withdrawing from friendships, or abandoning hobbies and activities that were once important. The pursuit and use of the drug take precedence, leading to a cascade of negative consequences in one’s personal, social, and professional life.
Health Effects of Xanax Misuse
The long-term, non-medical use of Xanax can result in a wide array of adverse health consequences that affect cognitive function, mental stability, and physical well-being. These effects often develop insidiously over time and may not be immediately attributed to the medication itself.
Understanding these risks is vital, as many are partially or fully reversible with professional treatment and sustained abstinence.

Mood Changes and Irritability
While Xanax is prescribed to mitigate anxiety, chronic misuse can have a paradoxical effect, leading to increased irritability, agitation, and unpredictable mood swings.
Some users report a state of emotional blunting or anesthesia, where they feel detached from their feelings and unable to experience a normal spectrum of emotions, both positive and negative. This occurs as the drug’s constant presence on GABA receptors disrupts the brain’s delicate and natural systems for emotional regulation.
Memory, Attention, and Reaction-Time Problems
Benzodiazepines are well-documented to cause significant cognitive side effects. Long-term use frequently impairs anterograde memory, which is the ability to form new memories. This can make it difficult to learn new information or recall recent conversations and events.
Chronic use also leads to deficits in concentration, sustained attention, and information processing speed. Critically, it slows reaction times, which impairs motor coordination and makes operating machinery or driving a vehicle extremely dangerous.


Insomnia and Other Sleep Disruptions
Although Xanax induces drowsiness and is sometimes misused as a sleep aid, it fundamentally disrupts healthy sleep architecture. It suppresses the deeper, more restorative stages of sleep (slow-wave sleep and REM sleep).
Over time, this leads to a state of dependence for sleep initiation, where the patient feels unable to fall asleep without the drug. Upon cessation, a severe rebound insomnia often occurs, which can be more intense than the initial sleep problems, reinforcing the cycle of use.
Verified Credentials and Treatment Standards at Lost Angels
Lost Angels operates under formal oversight through licensure with the California Department of Health Care Services (DHCS) in California (license or registration number 191512AP) and accreditation from The Joint Commission, which aligns the program with standardized expectations for safety, quality, and clinical operations.
In addition, Lost Angels maintains a verified Psychology Today profile and a Better Business Bureau business profile, offering third-party reference points that patients and families can review when evaluating treatment options.


Find a Professional Xanax Rehab in Los Angeles
Choosing Xanax rehab in Los Angeles is often less about a single decision and more about finally getting honest support for a complicated situation. Lost Angels can help you sort through symptoms, risks, and next steps with an experienced clinical lens.
If you’re ready to seek treatment, you can contact Lost Angels to talk about a plan that supports both stabilization and healing. You deserve care that recognizes benzodiazepine dependence as treatable—and treats you with respect throughout benzodiazepine addiction recovery.
References
- Frontiers in Psychiatry – GABAA Receptor Subtypes and Benzodiazepine Use, Misuse, and Abuse
- Substance Use & Misuse – Evaluation of DSM-5 Diagnostic Criteria for Betel-Quid Use Disorder Using the Addiction Characteristics Defined by American Society of Addiction Medicine
- Psychology Today – Lost Angels Treatment Center Profile
- Better Business Bureau – Lost Angels Profile
Frequently Asked Questions
What Is The Process For Xanax Rehab Treatment In Los Angeles?
The process begins with a confidential assessment to understand your unique situation. This is followed by medically supervised detoxification to safely manage withdrawal. Afterward, you will transition into a personalized treatment program, which may be residential or outpatient, involving evidence-based therapies and holistic support. The final stage is comprehensive aftercare planning to support your long-term recovery.
How Long Does Xanax Rehab Typically Last In Los Angeles?
The duration of treatment is individualized. Medical detox usually takes 7 to 14 days. Residential inpatient programs typically last from 30 to 90 days, depending on clinical needs and progress. Following residential care, outpatient programs and aftercare support can continue for several months to reinforce recovery skills.
Does Xanax Rehab In Los Angeles Accept Insurance, And Which Plans Are Covered?
Most reputable Xanax rehab centers in Los Angeles accept PPO insurance plans. Our admissions team can provide a confidential verification of your benefits to determine what your specific plan covers. This service helps you understand any potential out-of-pocket costs, such as deductibles or co-pays, before you begin treatment.
Do Los Angeles Xanax Rehab Centers Offer Support For Co-Occurring Mental Health Disorders?
Yes, high-quality Xanax rehab programs provide integrated dual diagnosis care. This means they are equipped to treat co-occurring mental health conditions like anxiety, depression, or PTSD at the same time as the substance use disorder. This comprehensive approach is critical for achieving lasting recovery and overall well-being.
What Are The Most Effective Treatments For Xanax Addiction?
The most effective treatment is a comprehensive approach that starts with medically supervised detox. This is followed by a combination of evidence-based therapies like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT), individual and group counseling, dual diagnosis care for mental health, and robust aftercare planning. Treatment is most effective when it is personalized to the individual’s specific needs.
What Should I Bring Or Prepare For Entering Xanax Treatment In Los Angeles?
You should prepare by packing comfortable clothing, essential alcohol-free toiletries, your ID and insurance card, and a list of any current medications. It is important to leave valuables, non-essential electronics, and any outside food or substances at home. A detailed packing list will be provided by the admissions team to help you prepare.